Molluscum Contagiosum & Find Out More About This Growing Viral Skin Condition
There is a viral skin condition that is appearing more often and which has rather a strange name – it is called molluscum contagiosum.
As its name suggests, the virus is very contagious and easily spreads both from person to person and from one part of the body to another part of the same body.
A virus is a small infectious agent that can only replicate inside the cells of another organism. The word is from the Latin ''virus'' referring to poison and other noxious substances.
Molluscum can be mistaken for other skin conditions
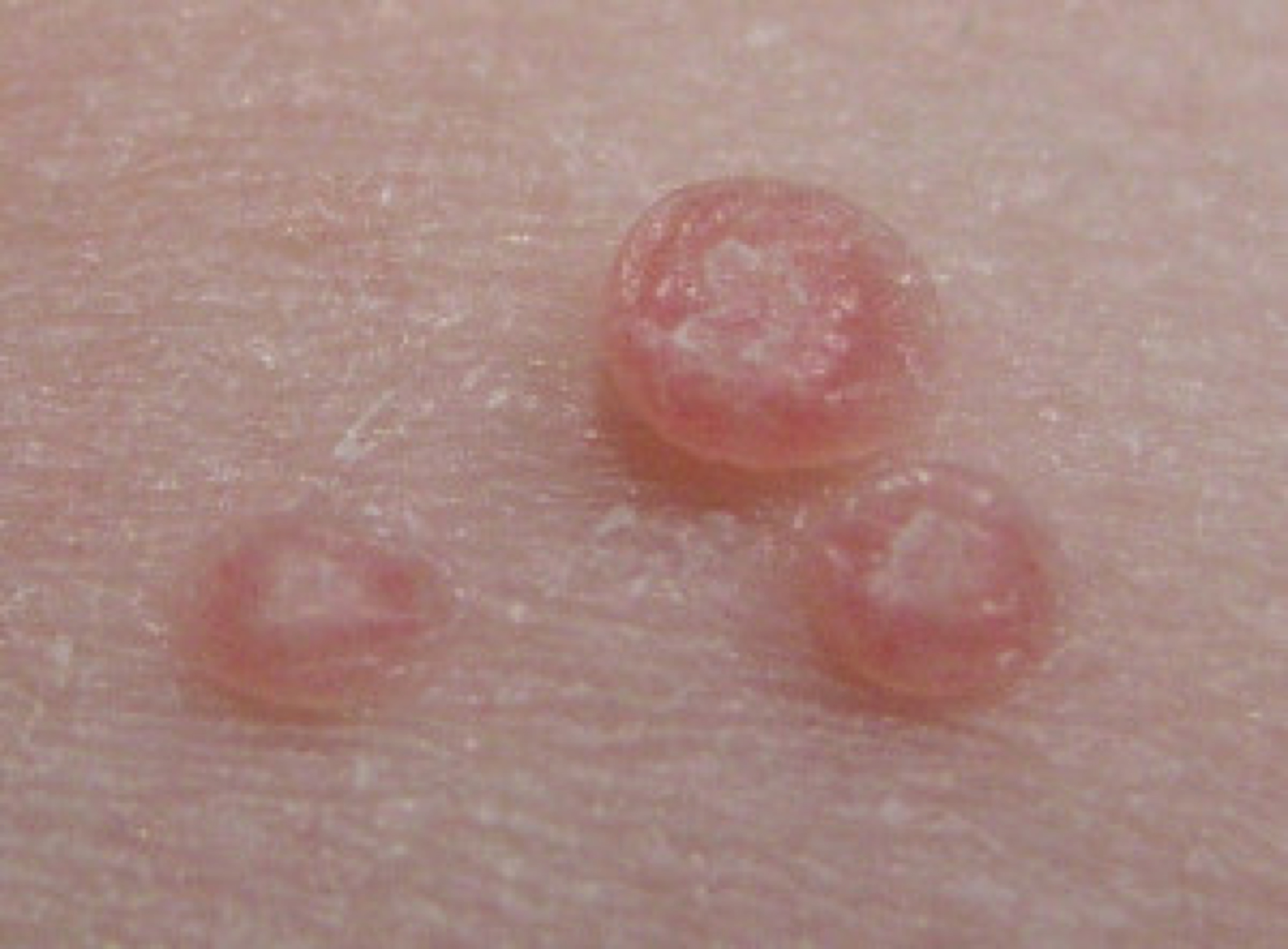
This contagious skin condition can often be mistaken for other skin conditions such as warts, chickenpox or shingles, herpes sores, basal cell skin cancer and lichen planus. The most common and distinguishing symptom of molluscum is the appearance of small lesions or bumps, which are often indented in the center. It is this indentation that greatly helps with a diagnosis.
Other symptoms include
- The lesions or bumps are firm and raised.
- The bumps are usually pearly and flesh-colored but may be either clear or red and inflamed.
- These bumps are normally about 0.1 inches to 0.2 inches in size – that is slightly smaller than a pencil eraser.
- These bumps are sometimes filled with a thick white material.
- They can appear alone or in a group. These groups (from just a handful to as many as 20 to 30) are often in one or two areas. Otherwise healthy children and adults will usually have no more than 20 lesions on their body.
Molluscum is almost like two different conditions
On the one hand it is a childhood disease that can be found in young children where the bumps usually appear on the body, face and arms, while on the other hand it often occurs in teens and young adults when the bumps appear in the groin area, genitals, inner thighs and spreading upwards over the abdomen.
In rare cases, lesions may develop in a number of other places in both adults and children including: palms of the hand, soles of the feet, inside the mouth or around the eyelid. Although these bumps are sometimes itchy, there is not usually any pain or other discomfort. Always avoid handling or squeezing the lesions because this can spread the infection to other parts of the body.
Unfortunately, molluscum can be quite long standing with the symptoms lasting for two to four months or even longer. Just as old lesions start healing, new ones can form as the virus spreads to new areas of the skin. As the body's immune system starts to fight the virus, the lesions can become crusted or scabby. An added complication (especially in children) is when patches of eczema develop around the molluscum bumps and lesions.
Eczema is a skin condition where the skin becomes itchy, reddened, dry and cracked. This is thought to happen because some people are particularly sensitive to the effects of the virus that is responsible for molluscum. Further, children who have atopic eczema (this is where the skin is particularly sensitive to substances such as dust mites or pollen) may be more vulnerable to this additional symptom. If you or your child have a history of eczema, then the molluscum can develop in tangent with the eczema rash so that the eczema is often more noticeable than the molluscum bumps.
The lesions do not usually leave scars, but you may notice that each one leaves a tiny patch of lighter skin or a tiny pitted mark.
The complication of a weakened immune system and molluscum
A problem can arise when those with a weakened immune system contract the virus especially if they are already suffering from another infection such as HIV or AIDS. The molluscum then becomes more serious and the signs and symptoms very apparent.
The risk of spreading the virus
Found throughout the world, molluscum is more common in hot and humid climates and incidence of this virus is increasing. As children usually play together in close proximity, it is easy for the virus to be spread from one child to another. It can also be spread: through sexual intimacy (in the case of adults); through sharing inanimate objects such as towels and clothing; by using swimming pools and sharing baths; or by scratching, rubbing or touching so that the virus spreads from one part of the body to another (this is called autoinoculation).
This virus does increase the risk for other skin infections.
Sources
Molluscum contagiosum. (2015)
healthychildren.org/English/health-issues/conditions/skin/pages/Molluscum-Contagiosum.aspx. (Accessed, 20 March 2021).
Molluscum contagiosum. (2015).
cdc.gov/poxvirus/molluscum-contagiosum/. (Accessed, 20 March 2021).
aad.org/public/diseases/contagious-skin-diseases/molluscum-contagiosum. (Accessed, 20 March 2021).